Blog
The Prescription to Evaluating Telemedicine Is Using a Holistic Framework

Telemedicine became an essential tool for delivering healthcare services remotely during COVID-19. But was this growing trend of virtual doctor visits truly effective, and will it continue post-pandemic? Current evaluation systems present many limitations to determining how well telemedicine is performing. A more comprehensive framework is needed to get the RX to success. Read on to find out what is needed.
With telemedicine adoption surging and gaining greater acceptance by physicians and patients, determining the quality of the services provided has become critically important. Moving ahead, providers must have satisfactory answers to such lingering questions as: How do you effectively evaluate telemedicine? What impact do all the stakeholders involved have in the evaluation? Are the current evaluations extensive enough to cover all factors?
While telemedicine usage skyrocketed due to the unavoidable circumstances of the pandemic and provided many immediate benefits, we now need to understand if its usage will continue in the long term as normalcy returns.
In comparison to in-person visits, telemedicine is more complicated, especially when considering the additional stakeholder responsibility involved from payers, providers, policymakers, technology providers, and consumers.
Beyond the care outcome that is usually gauged in typical face-to-face appointments, such factors as implementation, delivery, and repeatability must also be rated to determine the true value of telemedicine.
The need of the hour is creating better, extensive, and holistic evaluation frameworks that take into consideration most, if not all, of the dimensions that affect the overall care and patient experience delivered virtually.
Obstacles to overcome
Telemedicine evaluation frameworks and methodologies have been evolving. However, the sluggish rate of telemedicine adoption and skepticism toward its practice until now has delayed the progress in creating a more comprehensive evaluation framework.
Also presenting obstacles to a more holistic approach are the considerable variations in focus areas and the narrow and isolated scope of evaluation, such as those only considering specific clinical areas, measuring patient satisfaction, evaluating technology, assessing cost and efficiency, etc., separately.
While piecemeal evaluations catering to specific aspects of the telemedicine continuum help gauge a particular aspect, they cannot effectively capture the wider and more complex horizons of telemedicine.
A better holistic framework that encapsulates all evident and latent aspects starting from defining the needs of telemedicine care to measuring long-term health and experience outcomes is needed.
Telemedicine evaluation elements
Telemedicine providers need to look deeper than healthcare outcomes and consider the more abstract elements like patient and provider satisfaction, usability, and repeatability. The framework currently used by the Institute for a Broadband-Enabled Society (IBES) uses patient control, clinical quality of care, organizational sustainability, and technology capabilities as its factors.
Another example of a framework, which stems from academic roots, uses an assessment model looking at three dimensions based on functionality (consultation, diagnosis, monitoring, and mentoring), technology (modes, network design, and connectivity), and applications (treatment modalities, medical specialty, disease types, and sites). All such frameworks tend to take a certain perspective of a technological lens or care-outcome focused framework.
Six areas to consider when building or updating telemedicine evaluations
A framework for evaluation must span across the entire gamut of possible action points while looking at all the potential barriers and bottlenecks. The below framework attempts to cover the many diverse factors that are indispensable to telemedicine’s success.
Key Elements: Holistic Telemedicine Framework
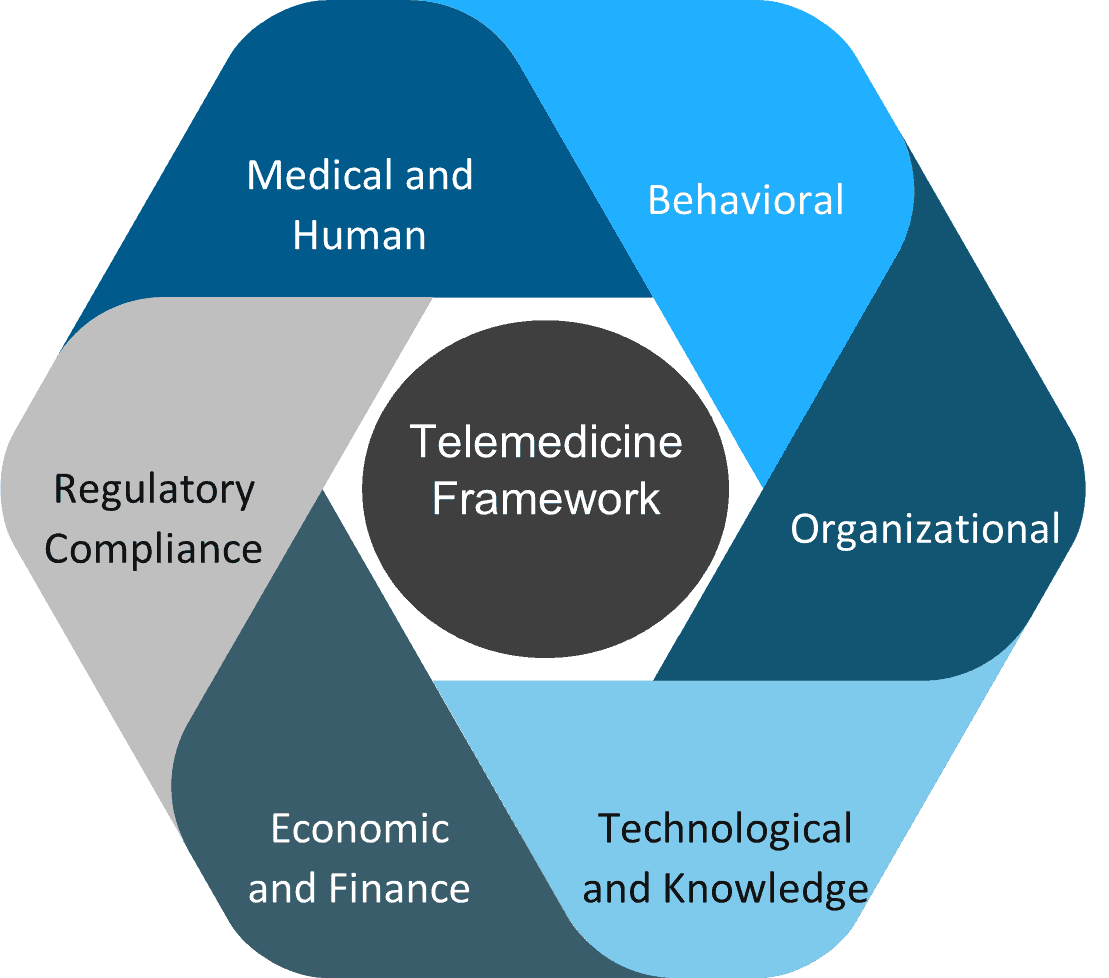
Everest Group (2021)
- Medical and human – This includes looking at health outcomes, the number and type of medical conditions, the nature of medical services provided (diagnosis, treatment, wellness advice, etc.), and the spectrum of care provided. Also to be evaluated are all the interacting human entities that play a part in healthcare delivery, such as provider staff and expertise, non-medical staff, technical teams, support, and maintenance personnel
- Behavioral – This covers the behavioral aspects of the patient/client and provider such as awareness, perception, satisfaction, acceptability, adaptability, and other elements that encompass how involved stakeholders respond and react to a telemedicine application should be rated
- Organizational – All aspects defining and involving care provider, patient, payer, administration, and technology structure need to be graded. This includes evaluating the leadership, organizational culture, workflows, hospital information systems, teams involved, etc.
- Technological and knowledge – Technology tools and the technical knowledge that enables telemedicine to thrive should be reviewed, including the information systems, databases, platforms, software, applications, security systems, and other technological infrastructures in use. Also to be rated are the knowledge constitutes of interoperability, data quality, systems speed/performance, maintenance, and support, etc.
- Economic – Elements relating to the economic and financial aspects that include financial performance, investment returns, financing business, and economic impact are all aspects to take into consideration
- Regulatory, legal, and compliance – Evaluation of resolutions involving reimbursements, state and federal laws, compliance, privacy issues, medical legalities, technological compliances, and other legal/regulatory issues are all factors to be looked at
Organizational leaders need to step back and look at the complex structure in addition to their individual functions to gain a holistic understanding and reach the larger goal of building a successful telemedicine practice.
By expanding the view to these key areas, organizations will gain a more accurate picture of the effectiveness of telemedicine and be able to determine whether it will be sustainable in everyday instances moving forward.
Everest Group’s recent research, Unpacking the Rise of Telehealth, captures key insights of the telehealth market, covering trends across adoption, technology, and service provider dynamics. Please drop us your thoughts and reach out to us for a conversation at [email protected] or [email protected].