Healthcare Payer BPS Activity by Buyer Size: Gradual Shift | Market Insights™

Healthcare payer BPS activity by buyer size: gradual shift

Healthcare payer BPS activity by buyer size: gradual shift

The healthcare payer business process services market grew about 10% over the past year, driven in part by a shift in payers’ demand from cost reduction to more strategic, value-creating initiatives
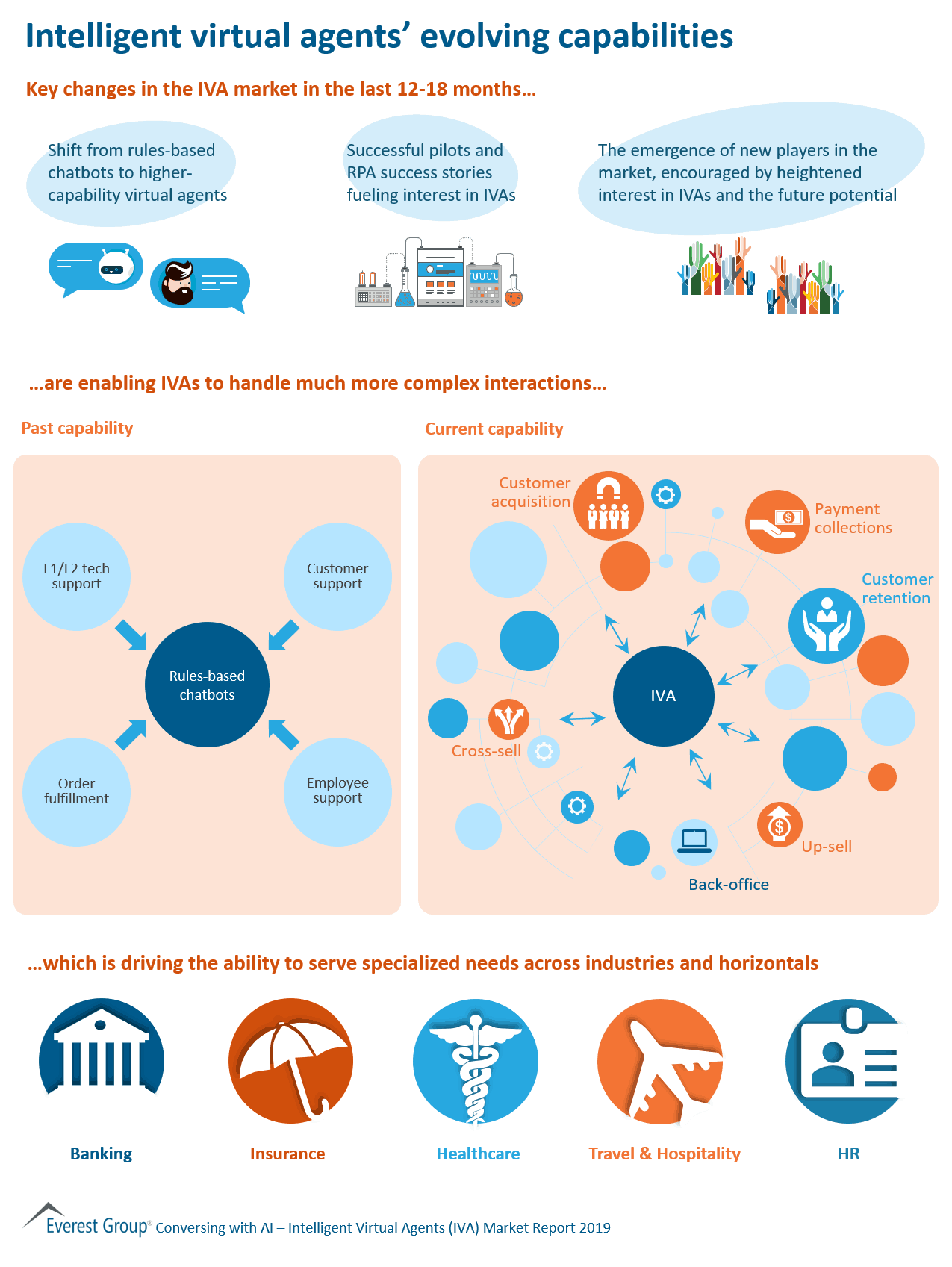
Intelligent virtual agents’ (IVA’s) evolving capabilities: Key changes in the IVA market in the last 12-18 months are enabling IVAs to handle much more complex interactions which is driving the ability to serve specialized needs across industries and horizontals
I experienced three pleasant surprises at last week’s Healthcare Information and Management System Society (HIMSS) conference. They were all about a perfect storm that is building to correct all that has been wrong in the digital healthcare space all these years.
Payers and providers alike are growing increasingly disillusioned with the outcomes of their digital programs. In fact, 78 percent of the healthcare leaders we surveyed in late 2018 indicated some sort of failure with their digital initiatives, whether big or small. The good news here is that most forward-thinking leaders are going back to the drawing board to redefine their digital strategy. Anthem, Intermountain Healthcare, and New York Presbyterian are great examples of organizations that have taken up the cudgels to fix digital healthcare where it fails – organization and culture.
To make the “patient experience” successful, enterprise leaders are taking a step back and focusing their attention on creating experiences for their workforce, clinicians, and partners (e.g., physician group, CMS, government agencies.) Don’t get me wrong, patients still need to be at the center of our universe. However, the personas that enable and deliver experience for patients need a fix first.
It was heartening to see the likes of Amazon, Google, Microsoft, and Salesforce steal the march from the big boys in the healthcare tech space – i.e., Cerner and EPIC – in asserting themselves as the technology visionaries in healthcare. Their focus on healthcare microservices is a relief for healthcare executives trying to navigate the “all or nothing” approach of the EMRs.
There is one player that seems keen on reinventing itself: Optum. Through a nimble product and services strategy, Optum is touching upon on all the hot buttons – MLR, analytics, PBM, and claims. Optum is the specialist vendor to watch out for when it comes to healthcare.
Last, but not least, what really took the cake were the innovative and exciting POCs related to clinical AI and visualization that Israel and Ireland – yes, the countries – showcased in their booths. These were some of the most fully baked solutions that I have seen in my 10 years attending HIMSS.
Hence, it’s with good reason that I left fairly impressed with the developing ecosystem knocking on the doors of healthcare organizations that are hungry for outcomes.
I will sign off by sharing an illustration from our recent study that analyzed the investments 27 of the leading healthcare payers and providers have made in artificial intelligence (AI), a key marker in the world of digital healthcare. This study objectively analyzed these investments from the perspective of ROI achieved.
As you can see, there is a wide variance even within such a small sample set of healthcare organizations. FOMO (Fear Of Missing Out) pushed a lot of organizations to invest in the flashy new toy called AI. However, not all of them embarked on their investment journey by first enabling the core components of capability.
The difference between the best and the rest in healthcare is simply this: the ones to get the best ROI – those on the top right – are taking their journey through step functions that enable not only technology but also an organizational culture of innovation.
Please contact me at [email protected] if you’d like to hear more about my take-aways from the HIMMS conference or our study, named “Dr. Robot Will See You Now: Unpacking the State of Artificial Intelligence in Healthcare – 2019.”
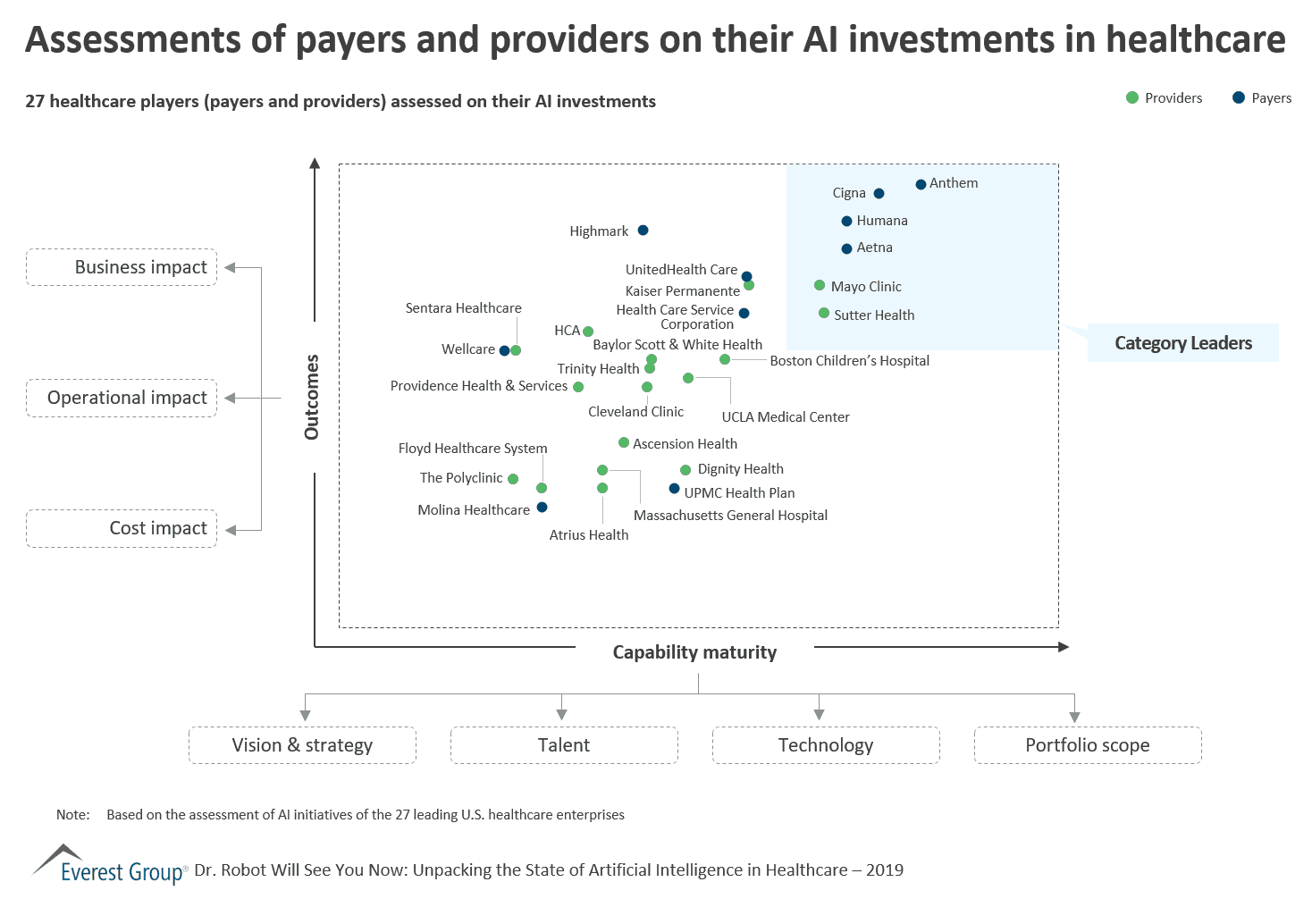
Assessments of payers and providers on their AI investments in healthcare: 27 healthcare players (payers and providers) assessed on their AI investments

The future looks promising for AI-based automation…but barriers that restrict its universal acceptance remain

While the explosion of data, cognitive overload, endless documentation, and user burnout in the healthcare industry are driving demand for AI, it has implications far beyond technology: the majority of AI decisions impact business processes, customer experience, and cost – key concerns for chief executives
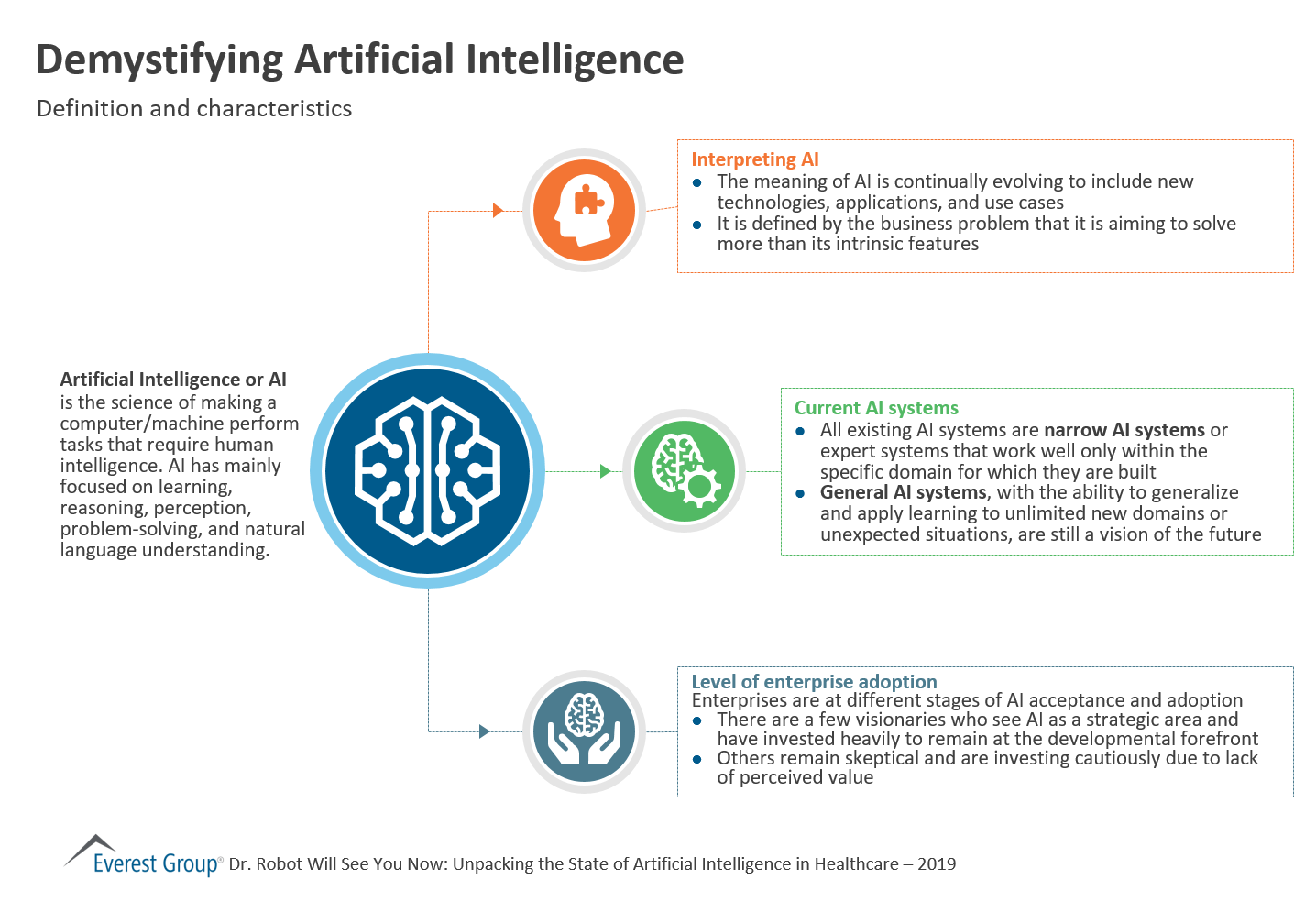
Demystifying Artificial Intelligence: Definition and Characteristics
New research predicts US$6 billion investment will drive innovations in patient identity verification, opioid abuse detection and individually tailored healthcare.
Healthcare organizations are pouring billions into embedded AI across the value chain, driving an estimated quadrupling of AI investments in the next three years, according to Everest Group. The firm predicts that healthcare AI investments will grow from US$1.5 billion in 2017 to exceed US$6 billion by 2020, representing a compound annual growth rate of 34 percent.
While AI is a relatively new area in the healthcare space and its adoption is in the nascent stage, digitalization of healthcare is accelerating healthcare enterprises’ interest in AI. AI has the potential to transform healthcare processes and dramatically reduce costs and improve efficiencies.
For example, healthcare payers are leveraging AI for product development, policy servicing, network management and claims management. Examples include:
Currently, the area where payers are adopting AI to the greatest extent is in care management.
Likewise, the highest adoption of AI by healthcare providers is for care and case management. Providers also are employing AI tools to:
These findings and more are discussed in Everest Group’s recently published report, “Dr. Robot Will See You Now: Unpacking the State of Artificial Intelligence in Healthcare – 2019.” The firm has analyzed the market from the vantage point of 27 leading healthcare enterprises and closely examined the distinctive attributes of the leaders, who are far ahead of the other industry participants in terms of AI capability maturity. The report identifies best practices, illustrates the impact generated, and offers proposed a roadmap for market stakeholders.
***Download a complimentary abstract of this report here. ***
“While healthcare enterprises are still in the nascent stages of AI adoption, the scale of opportunity in AI demands C-level vision,” said Abhishek Singh, vice president of Information Technology Services at Everest Group. “AI presents unique opportunities for healthcare enterprises – allowing them to improve customer experience, achieve operational efficiency, enhance employee productivity, cut costs, accelerate speed-to-market, and develop more personalized products. In the case of the leading healthcare organizations, their CEOs and CIOs are acknowledging the transformative power of AI, rapidly building appropriate AI strategies, and building a robust, overarching business plan to harness its benefits.”
Additional key findings:
Indian IT services major Wipro may have to look at building solutions beyond healthcare enrolment-based services for its Health Plan Services unit to remain competitive amid legislative changes in the US, say analysts.
The Donald Trump-led US administration has pushed consistently to repeal Obamacare, which extended health insurance benefits to a large chunk of low-income people in the US.
At this juncture, Wipro should look “to double down quickly (to) address the re-pivot issues,” Peter Bendor-Samuel, chief executive of global IT advisory firm Everest Group, told ET.

©2023 Everest Global, Inc. Privacy Notice Terms of Use Do Not Sell My Information
"*" indicates required fields